Uterine Cancer
 There are two main types of uterine cancer. Uterine cancers begin in the lining of the uterus (endometrium) and account for about 95% of all cases. Uterine sarcomas are a rarer form of uterine cancer that develop in the muscle tissue (myometrium).
There are two main types of uterine cancer. Uterine cancers begin in the lining of the uterus (endometrium) and account for about 95% of all cases. Uterine sarcomas are a rarer form of uterine cancer that develop in the muscle tissue (myometrium).
Uterine cancer is the most commonly diagnosed gynaecological cancer in Australian women. Due to an early warning symptom (abnormal uterine/vaginal bleeding) the vast majority of patients with uterine cancers are diagnosed at an early stage.
- An estimated 3,493 women will be diagnosed with uterine cancer in Australia in 2025;
- Uterine cancer remains as the fifth most commonly diagnosed cancer among females;
- Approximately 706 women will die from uternine cancer in 2025;
- The 5-year survival rate (2017-2021) for uterine cancer is about 82.5%. Patients with high-risk uterine cancer (ie. uterine papillary serous carcinoma) have a lower chance of survival.
Uterine cancer symptoms
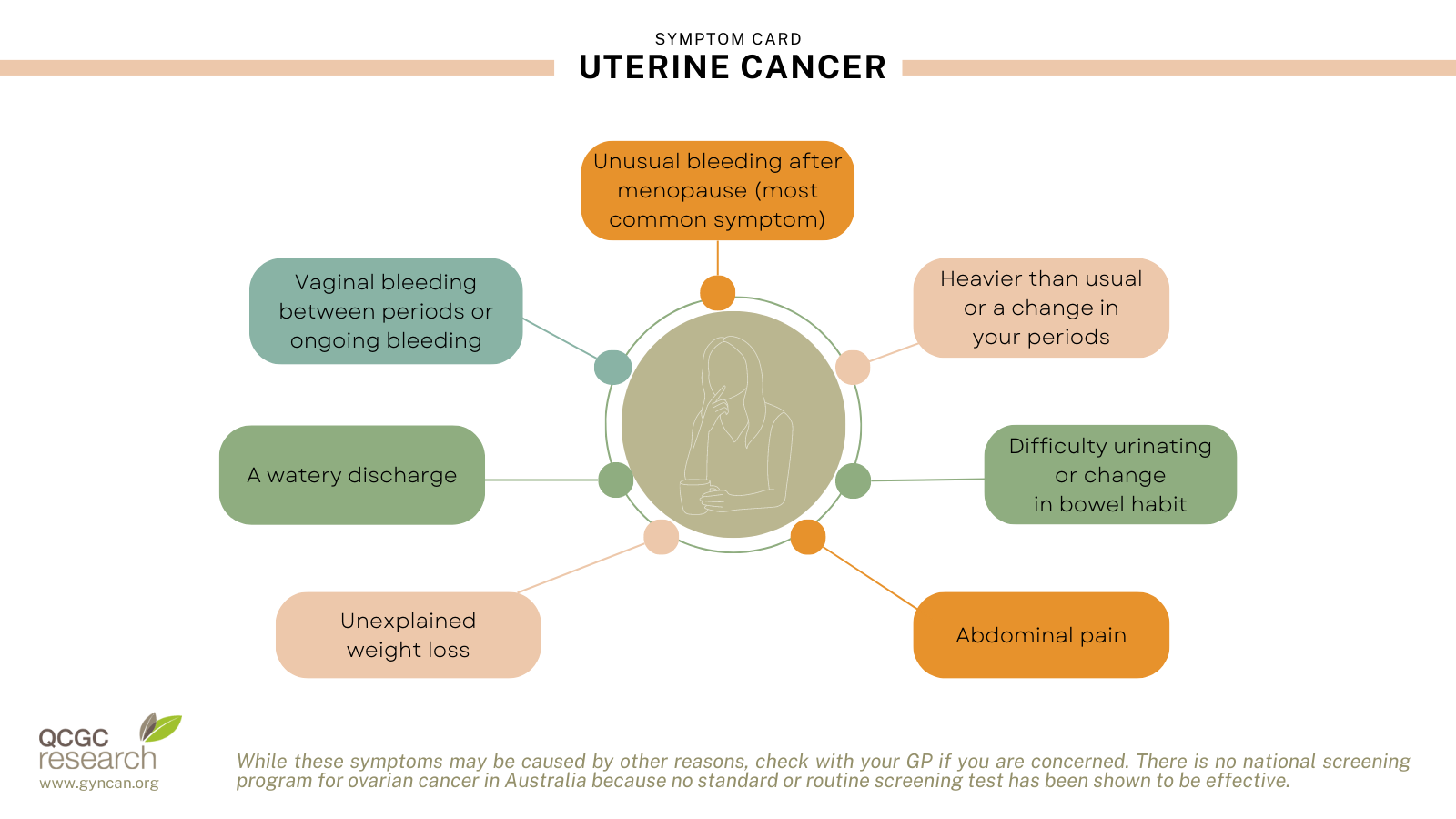
Uterine sarcoma symptoms
- bleeding between periods
- bleeding after menopause
- a mass or lump in the vagina
- pain or a feeling of fullness in the abdomen (belly)
- frequent urination
Known risk factors
Some factors can increase your risk of uterine cancer:
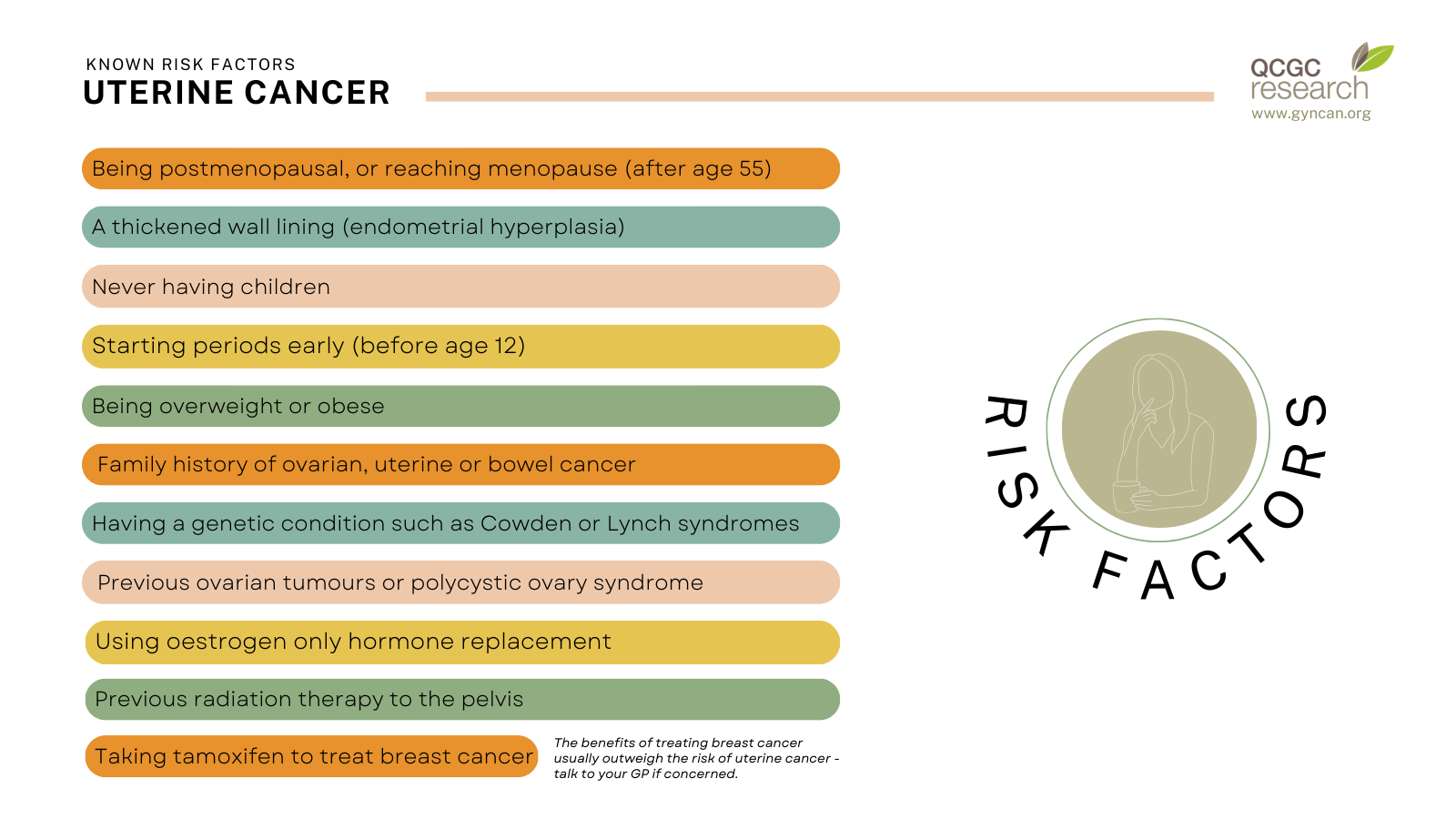
There are no proven measures to prevent uterine cancer. However, you may be able to minimise your risk factors, such as maintaining a healthy weight, and being vigilant about any abnormal vaginal bleeding.
Screening
Diagnosis and Treatment
Standard treatment is a full hysterectomy, removal of both fallopian tubes and the ovaries. The extent of the disease will be determined by preoperative imaging and removal of lymph nodes along the large blood vessels in the pelvis. Most patients do not require postoperative treatment. However, patients at higher risk of relapse are recommended to have chemotherapy, radiotherapy or a combination of both, depending on the cell type and extent of the disease.
See the Cancer Australia website for more information on diagnosis testing and treatment options.
The Cancer Council also provides a "Endometrial Cancer: Your guide to best cancer care" which explains the standard of high-quality cancer care that all Australians can expect, from diagnosis, to treatment, recovery, and living with cancer.
Research
Current research focuses on less invasive surgical techniques, which may lead to improved recovery from surgery with equal chances for survival. For patients with high-risk uterine cancer, we are trying to find combinations of treatment (including new biological agents) to improve survival.
Click through to see more information on our endometrial cancer research:
Sources: Cancer Australia; Cancer Council




