LACC Trial
 This trial officially closed to recruitment in December 2017.
This trial officially closed to recruitment in December 2017.
The LACC Trial recruited 631 patients worldwide. The findings to date have captured the medical and scientific world’s attention. Analysis is ongoing as many of our patients have yet to reach the 4.5 year follow up timepoint.
Important news about the LACC trial was released in November 2018 by UQ's QCGC Research - read more in the below two articles:
- Q&A: What happens when you discover unexpected results in research
- Laparoscopic hysterectomies not the answer for cervical cancer
Anyone wishing to know more about the trial findings and how it may affect them, is advised to contact the gynaecology oncology case manager of your public hospital or your surgeon’s office if you are a private patient.
Global Influence - Invitations to speak at international conferences about the LACC Trial:
Quality of Life - LACC Slides - IGCS Kyoto 2018
LACC presentation - Adverse events - IGCS 2018
LACC Presentation - SGO March 2018
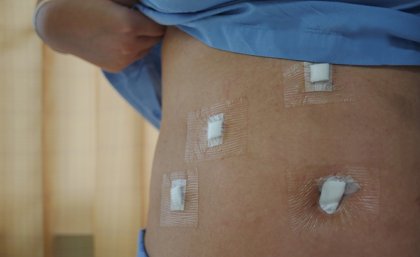 A phase III randomised clinical trial of laparoscopic (keyhole) or robotic hysterectomy versus adominal radical hysterectomy in patients with early stage cervical cancer. Focusing on Post-Op Recovery, Quality of Life, Recurrence rates and Long Term Disease Free Survival between the two treatment options.
A phase III randomised clinical trial of laparoscopic (keyhole) or robotic hysterectomy versus adominal radical hysterectomy in patients with early stage cervical cancer. Focusing on Post-Op Recovery, Quality of Life, Recurrence rates and Long Term Disease Free Survival between the two treatment options.
Cervical cancer is the most common cause of death from gynaecological cancer world-wide. In developed countries with an excellent public health infrastructure and a high compliance of women, early cytological detection of cervical cancer (PAP smear) has led to an impressive reduction of mortality while in other world regions including Central America, South East Africa and India, incidence and mortality rates are still very high. Today, more than 80 per cent of all cervical cancer deaths occur in developing countries. However, the number of cases estimated to be diagnosed with cervical cancer every year is an alarming 14,000 in the USA, 58,000 women in Europe and 2000 in Australia and New Zealand (International Agency for Research on Cancer, Globocan WHO 2012).
Currently the standard treatment option for women with early stager cervical cancer is a Total abdominal radical hysterectomy (TARH - removal of uterus, the upper one to two cm of the vagina and the soft tissues around the cervix are excised) and pelvic lymph node dissection (± aortic lymph node dissection ± postoperative chemo- radiotherapy). While this is an accepted effective treatment, a laparotomy is highly invasive, visibly scarring and is associated with higher treatment related morbidity[i] [ii]. Additionally, radical hysterectomy by laparotomy is associated with an average hospital stay of approximately 5 to 7 days and an average recovery period (from surgery) of 5 to 6 weeks.
The LACC Trial aims to compare the above standard treatment against minimally invasive surgery (MIS) via TLRH/TRRH - Total Laparoscopic or Total Robotic Radical Hysterectomy which is effectively the same operation as above yet done via smaller incisions into the abdomen.
Laparoscopic techniques have been demonstrated to be feasible and safe with previous retrospective studies on TLH (Total Laparoscopic Hysterectomy) showing encouraging results[iii]. In a number of retrospective and prospective, non-controlled series the incidence of treatment-related morbidity was less in patients who had a laparoscopic hysterectomy compared to patients who underwent a TAH (Total Abdominal Hysterectomy)[iv]. Hospital stays are generally much shorter usually 2-3 days. Retrospective data suggest that the recurrence rate and patterns of recurrence are similar in patients who had a laparoscopic or an open approach[v].
The Primary outcome for this trial is disease free survival with secondary outcomes looking at:
Recurrence, Morbidity, Treatment costs, Quality of Life, Pelvic Floor function, Overall Survival at 4.5 years follow-up and the Feasibility of sentinel lymph node biopsy in this group of patients
The LACC Trial has recruited patients from multiple hospital/centres worldwide, with a cohort aim of 740 patients.
[i] Manolitsas TP, McCartney AJ: Total laparoscopic hysterectomy in the management of endometrial carcinoma. J Am Assoc Gynecol Laparosc 9: 54-62, 2002
[ii] Obermair A, Manolitsas TP, Leung Y, Hammond IG, McCartney AJ: Total Laparoscopic Hysterectomy vs. Total abdominal hysterectomy for obese women with endometrial cancer. Int J Gynecol Cancer. 2005 Mar-Apr; 15(2):319-24.
[iii] Obermair A, Manolitsas TP, Leung Y, Hammond IG, McCartney AJ: Total laparoscopic hysterectomy for endometrial cancer: patterns of recurrence and survival. Gynecol Oncol 92: 789-793, 2004
[iv] Obermair A, Manolitsas TP, Leung Y, Hammond IG, McCartney AJ: Total laparoscopic hysterectomy for endometrial cancer: patterns of recurrence and survival. Gynecol Oncol 92: 789-793, 2004
[v] Obermair A, Manolitsas TP, Leung Y, Hammond IG, McCartney AJ: Total laparoscopic hysterectomy for endometrial cancer: patterns of recurrence and survival. Gynecol Oncol 92: 789-793, 2004
